There is hot debate among healthcare professionals and legislative bodies over who can perform dry needling and who should perform dry needling. Learn the APTA’s stance on the issue here.
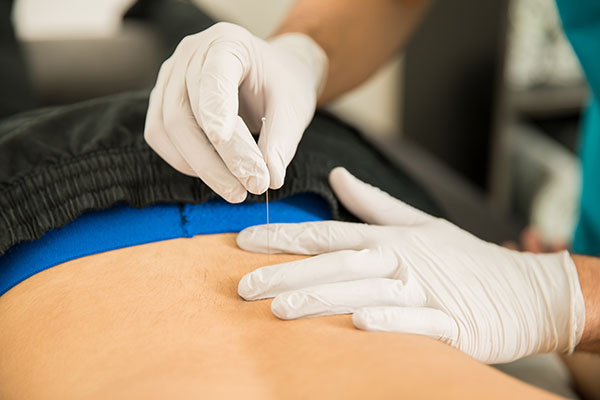 In our previous blog, we addressed the safety and efficacy of dry needling technique for treating a wide variety of acute and chronic pain conditions. But, exactly who can perform dry needling? That is, is dry needling within the scope of practice for all physical therapists or is special training required? And, should acupuncturists be able to perform this technique? In this blog, we answer these questions and more as we expound on the APTA’s (American Physical Therapy Association) and the FSBPT’s (The Federation of State Boards of Physical Therapy) recommendations as well as address common billing issues surrounding this treatment.
In our previous blog, we addressed the safety and efficacy of dry needling technique for treating a wide variety of acute and chronic pain conditions. But, exactly who can perform dry needling? That is, is dry needling within the scope of practice for all physical therapists or is special training required? And, should acupuncturists be able to perform this technique? In this blog, we answer these questions and more as we expound on the APTA’s (American Physical Therapy Association) and the FSBPT’s (The Federation of State Boards of Physical Therapy) recommendations as well as address common billing issues surrounding this treatment.
Who Can Perform Dry Needling?
In most clinical practice settings, an acupuncturist performs acupuncture while a physical therapist performs dry needling, which leads to the second question…
Should Physical Therapists Perform Dry Needling?
There is a huge controversy even among physical therapists on who can perform dry needling and more importantly – who should perform dry needling – within their own practice. Those who are in favor of dry needling are typically PTs who have seen positive results from using the technique on their patients for pain management. On the other side, there are therapists who feel other noninvasive pain management techniques are more advantageous.
To further complicate matters, there is strong opposition from acupuncturists in every state in regards to the practice of dry needling as it is very closely related to their own acupuncture practice and ultimately impedes business revenues.
It is good to remember that even if a PT chooses to perform dry needling, it is usually combined with other manual therapy techniques, stretching or strengthening exercises, a home exercise program, or additional modalities. Rarely is dry needling performed solo. Regardless, it is ultimately the therapist’s clinical judgment to evaluate and develop an appropriate treatment plan for his or her patient.
What is the PT’s Scope of Practice for Dry Needling?
Each state board has different requirements regarding therapists’ ability to perform dry needling. In 2012, there were 27 states that allowed dry needling practice within the scope of physical therapy practice.
The majority of states concur with the APTA’s stance that dry needling is not included in the physical therapist’s entry-level education. Therefore, a therapist is required to obtain advanced level continuing education or other formal training on dry needling technique. This is to ensure that the insertion of the needles is performed correctly and carefully. For example, per the Virginia State Board of Physical Therapy rules: “A physical therapist using dry needling must complete at least 54 hours of post-professional training, including providing evidence of meeting expected competencies that include a demonstration of cognitive and psychomotor knowledge and skills.”
Other examples of dry needling restrictions include Kansas, which up until recently (2016) did not allow PTs to perform dry needling: “Under Kansas dry needling regulations, dry needling can only be performed by licensed PTs, shall not be delegated, and can be performed solely for conditions and impairments that fall under the Kansas PT scope of practice.”
Currently, only 4 states consider dry needling outside the scope of practice for PTs: California, Utah, New York, and Hawaii.
Since every state board has different rules on dry needling within the PT’s scope of practice, it is recommended that physical therapists check with their own state board before incorporating this technique into their daily practice. This is especially important in states where dry needling is prohibited and/or continuing education or specialized training is required.
What are the Billing Issues PTs Face When Performing Dry Needling?
For billing purposes, it is important to note that dry needling is also known as intramuscular manual therapy, trigger point dry needling, or intramuscular needling. The APTA encourages the use of the terminology “intramuscular manual therapy” to describe the intervention.
Even though the APTA and FSBPT consider “intramuscular manual therapy” a method of treatment provided by PTs for pain management, there is currently no separate CPT code to bill for this procedure. At present, the APTA identifies “intramuscular manual therapy” as a type of manual therapy technique, and therefore, should be billed under the manual therapy CPT code.
There are some insurance companies who refuse to pay for dry needling services. As per the APTA’s advice, a PT should always check with the insurance company’s policy prior to providing treatment.
For physical therapists or other healthcare professionals who are interested in learning more about dry needling, see our continuing education course, An Introduction to Trigger Point Dry Needling.
References:
- https://www.fsbpt.org/download/forum_summer2012_stateofjurisdictions.pdf
- http://www.apta.org/StateIssues/DryNeedling/
- http://www.apta.org/uploadedFiles/APTAorg/Advocacy/State/Issues/Dry_Needling/TXAttorneyGeneralDryNeedling_052016.pdf
- http://www.apta.org/PTinMotion/2015/5/DryNeedling/
- https://www.fsbpt.org/Portals/0/Forum_Winter2016_DryNeedling.pdf
- https://www.fsbpt.org/Portals/0/documents/free-resources/Dry_Needling_Final_Report_Clean.pdf

 Call
Call