Use the guide below to educate family members and caregivers on the proper positioning for stroke patients.
 Proper anatomical positioning for stroke patients is important not only to reduce the chances of shoulder subluxation, but also to promote body awareness. As a result, proper positioning encourages the use of the neglected extremity after the stroke. Furthermore, extremities positioned correctly in supine as well as in sitting position will enhance stroke recovery and help regain motor control more rapidly.
Proper anatomical positioning for stroke patients is important not only to reduce the chances of shoulder subluxation, but also to promote body awareness. As a result, proper positioning encourages the use of the neglected extremity after the stroke. Furthermore, extremities positioned correctly in supine as well as in sitting position will enhance stroke recovery and help regain motor control more rapidly.
Educating Caregivers on Positioning for Stroke Patients
Providing education to caregivers regarding anatomical positioning will ensure correct body alignment for the patient, especially when the rehab team is not present in the facility or home. The following information can be printed and provided to family members and other caregivers as a reference. You can also copy the picture and place it in a resident’s room for simple instruction.
Positions to Facilitate:
Upper Extremity | Lower Extremity |
|
|
|
|
|
|
|
|
Positions to Avoid to Minimize Contractures:
Upper Extremity | Lower Extremity |
|
|
|
|
|
|
|
|
|
|
Supine Position:
|
|
|
Side-Lying Position:
Upper Extremity | Lower Extremity |
|
|
| |
|
Below is a picture which shows an example of proper positioning for stroke patients using pillows in the side-lying position. (The bold color is the affected side.)
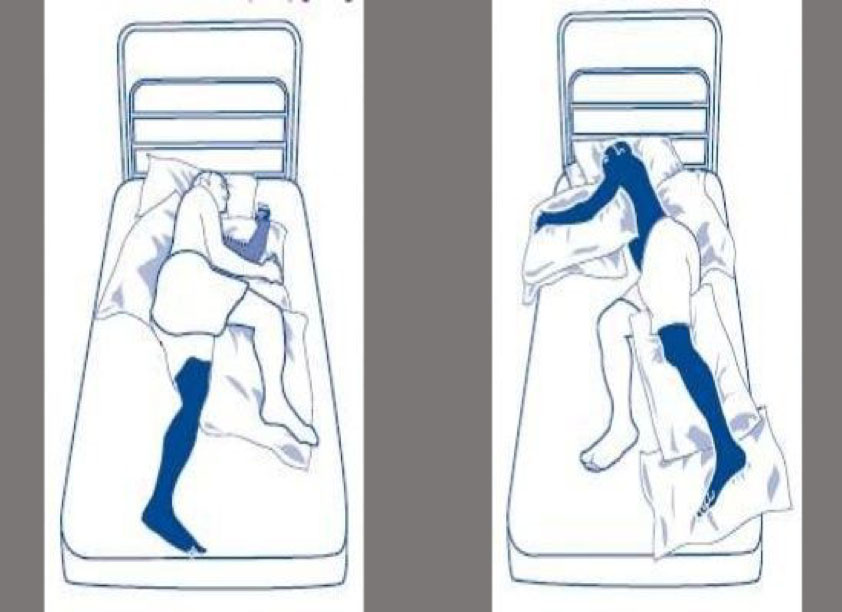
Lying on Unaffected Side:
|
|
|
|
|
Sitting Position:
In Bed | In Chair |
|
|
Examples of adaptive equipment to support the hemiplegic side are:
- Arm tray
- Foot box
- Lateral support around the lower back or on the footrest area of a wheelchair
- Foot pedal
- Lateral pads around thigh areas
- Adjustableheadrest
- Facial pad (for cervical dystonia)
- Wedges to support weaker areas and facilitate upright sitting
Learn More:
- Caring for the Stroke Patient
- Stroke in the LTAC and Home Health Setting
- Clinical Effects and Considerations of Stroke Based on the Affected Region of the Brain
References:
- Jong LD, Nieuwboer A, Aufdemkampe G. Contracture preventive positioning of the hemiplegic arm in subacute stroke patients: a pilot randomized controlled Clinical Rehabilitation. 2006; 20 (8).
- Ada L, Goddard E, McCully J, Stavrinos T, Bampton J. Thrifty Minutes of Positioning Reduces the Development of Shoulder External, Rotation Contracture After Stroke: A Randomized Controlled Arch Phys Med Rehabilitation 2005; 86: 230 – 234.
- Winstein CJ, Stein J, Arena R, Bates B, Cherney LR, Cramer SC, Deruyter F, Eng JJ, Fisher B, Harvey RL, Lang CE, MacKay-Lyons M, Ottenbacher KJ, Pugh S, Reeves MJ, Richards LG, Stiers W, Zorowitz RD; on behalf of the American Heart Association Stroke Council, Council on Cardiovascular and Stroke Nursing, Council on Clinical Cardiology, and Council on Quality of Care and Outcomes Research. Guidelines for adult stroke rehabilitation and recovery: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. 2016;47:e98–e169. DOI: 10.1161/STR.0000000000000098.
- Luzia G, Corinne J, Gilberto B, Robert T, Fred M. Motor Imagery training improves precision of an upper limb movement in patients with NeuroRehabilitation. 2015; 36 (2):157-166.
- Davis One- side Neglect: Improving Awareness to speed Recovery. Stroke Connection Magazine. 2003.
- Pollock A, Farmer SE, Brady MC, Langhorne P, Mead GE, Mehrholz J, Wijck FV. Interventions for improving upper limb function after Cochrane Reviews. 2013; DOI: 10.1002/14651858.CD010820.
- Rowat What do nurses and therapists think about the positioning of stroke patients? Journal of Advanced Nursing. 2001; 34 (6): 795-803.

 Call
Call
Leave a Reply