Rehabilitation during and after COVID-19 hospitalization is a key component in the continuum of care.
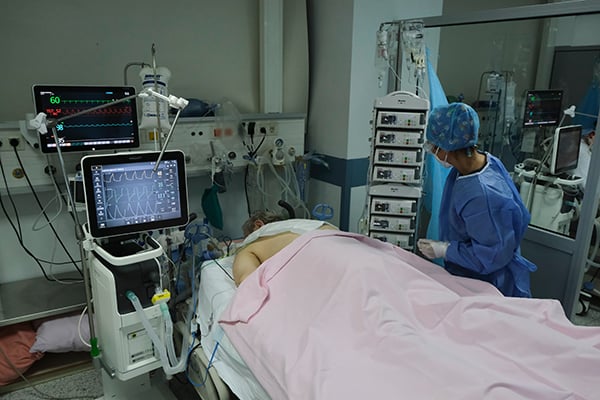
Though the benefits of proning far outweigh the risks, placing patients in this position may put them at risk for complications such as pressure injuries, airway complications, facial injuries, peripheral nerve injuries, musculoskeletal injuries, and cognitive impairment. In fact, affected patients may have long-lasting impediments towards functional recovery without proper rehabilitation intervention. Thus, multidisciplinary rehabilitation during and after hospitalization due to COVID-19 is a key component in the continuum of care.
Neurological & Musculoskeletal Conditions
Due to prolonged immobility, critically ill patients with COVID-19 are at risk for a multitude of neurological and musculoskeletal conditions including critical illness polyneuropathy and critical illness myopathy, ventilator-induced diaphragm dysfunction, ICU-acquired weakness, postural instability, muscle atrophy, and contractures (myogenic, neurogenic, and arthrogenic). In particular, shoulder and hip contractures have been reported as complications of prone positioning.
Some of these secondary complications can be anticipated in critically ill and immobilized patients and are therefore preventable with proper rehabilitation. For example, passive therapy is an important intervention that can mitigate the adverse effects of prolonged immobility and maintain the integrity of the musculoskeletal system.
Brachial Plexus Injuries
Brachial plexus injuries often develop in patients whose shoulders are positioned in abduction with external rotation and posteriorly displaced. This position causes compression and stretching of the brachial plexus, usually affecting the upper nerve roots or trunk. Preventive efforts with proper positioning can reduce the risk of brachial plexus injury. Post-proning rehabilitation should focus on mobility, strengthening, pain management, and addressing impairments related to activities of daily living or prior occupation.
Pressure & Facial Injuries
Risk factors for the development of prone-related pressure injuries include high body mass index (>28.4 kg m2), male sex, and age greater than sixty. During proning, the multidisciplinary team should regularly perform detailed skin assessments including examination for fascial injuries. Proper wound care and offloading techniques should be implemented including the use of silicone face foams and other head and neck supports. Early enteral nutrition has also been found to be safe; however, patients should be monitored for signs of aspiration, vomiting, or intolerance due to impaired gut motility. Therapy sessions to educate patients on compensatory swallowing techniques and safely advancing a patient’s diet are crucial for the timely restoration of function.
Cognitive Impairment & Delirium
Impairment of cognitive function and delirium are common in ICU patients. Studies have shown that ICU delirium is associated with increased mortality, prolonged hospitalization, prolonged mechanical ventilation, costs and the occurrence of cognitive disorders after discharge from ICU. Long-term cognitive impairments include problems with memory, attention and high-order executive functions.
The tools available for ICU delirium screening and diagnosis are validated tests available for all members if the medical team (physicians, nurses, physiotherapists). Their use for routine patient assessment is recommended by international medical and scientific societies. They have been implemented as Pain, Agitation, Delirium (PAD) Guidelines by the Society of Critical Care Medicine. Apart from monitoring, a strategy of prevention and treatment is recommended based on a non-pharmacological approach (restoration of senses, early mobilization, physiotherapy, improvement in sleep hygiene and family involvement) as well as pharmacological treatment (typical and atypical antipsychotics and dexmedetomidine).
Rehabilitation During and After Critical Illness
Up to two-thirds of survivors of critical illness face long-term problems as a result of their acute illness, the associated therapies, and their pre-existing chronic conditions. These problems include physical, cognitive, and mental impairments that have collectively been termed PICS (Post-Intensive Care Syndrome). PICS has widespread consequences after hospital discharge, including difficulty with self-care, decreased quality of life, and difficulty returning to work or social activities, all of which contribute to detrimental long-term health outcomes. Therefore, rehabilitation after critical illness is a key component in the continuum of care and should be delivered by multidisciplinary specialists including physical therapists, occupational therapists, speech therapists, dietitians, and counselors.
References:
1. Am J Phys Med Rehabil. 2020 Jun;99(6):470-474.
2. Am J Phys Med Rehabil. 2020 Jul 9:10.
3. Crit Care Med. 2007 Jan;35(1):139-45.

 Call
Call