How to Read a Knee MRI: An OT’s Perspective
Knee injuries can affect any age group. Knee injuries encompass a wide spectrum of trauma and conditions affecting one of the body’s most intricate joints. Ranging from mild strains to severe ligament tears and cartilage damage, knee injuries often result from sudden impacts, repetitive stress, or degenerative changes over time. Knee injuries can affect any […]
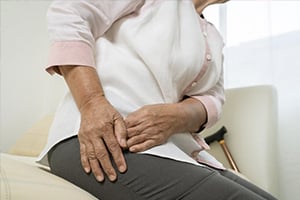
Read MoreHip Osteoarthritis: Rehab and Treatment Strategies
It’s also important to measure balance performance and activities that predict the risk of falls in adults with hip osteoarthritis. What is hip osteoarthritis (OA)? Hip osteoarthritis (OA) is a common disease with symptoms including joint pain, joint stiffness, and joint swelling. OA can result in functional impairment in daily activities, like walking, stair climbing, squatting, […]
Read MoreOccupational Therapy Continuing Education: The New Role of Technology
Let’s explore the exciting ways technology can transform Occupational Therapy CE. About 82.9% of clients report satisfaction with how occupational therapists use digital assistive technology (DAT) during their sessions. But DAT is just one example – the field is embracing technology in many ways. New and exciting technology tools can revolutionize how occupational therapists learn. […]
Read MoreSTIs, HIV, and Massage Therapy
By understanding the pathology and transmission of HIV and common STIs, massage therapists can help alleviate their client’s feelings of isolation. Massage therapy is generally safe for both clients and therapists, as the risk of HIV or STI transmission is very low without the exchange of bodily fluids. However, following basic safety rules, like discussing […]
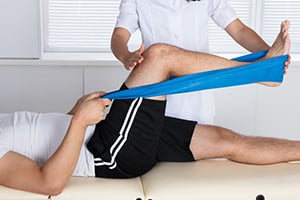
Read MoreRunning Injury Recovery: Helping Athletes Return to Sport
When planning a return to running, psychological readiness is equally as important as physical readiness. Returning to sport after a running injury requires a cautious and systematic approach to ensure the athlete’s full recovery and prevent further injuries. Although each athlete’s injury and recovery are different, a general step-by-step approach can help to develop and […]
Read MoreA PT’s Guide to Rehabilitation After ACL Surgery
People of all ages, physical conditions, and abilities can tear an ACL. A complex set of tendons and ligaments help stabilize and support the knee joint with its every movement, from a simple walking step to a cheerleader jump. Unfortunately, these tissues are vulnerable to injury. One of the most common knee injuries is an […]
Read MoreHip and Knee Rehabilitation for the Physical Therapist
Different standardized tests are helpful when assessing the functional ability and fall risk in a patient. Hip pain and knee pain are very common reasons for patients to seek physical therapy. Many different conditions can cause pain in the hip and/or knee. Often, patients with more chronic conditions have pain in both areas, and bilateral […]
Read MoreRehabilitation for Common Running Injuries
Running-related injuries aren’t all equally prevalent for every runner. Running injuries occur at all age ranges and skill levels, making them unique from patient to patient. Physical therapists aren’t just responsible for rehabilitating the injury itself. They also play a vital role in returning patients to pain-free running in the long term with preventative strategies. […]
Read MoreHow Do I Renew My Physical Therapy License in Michigan?
A quick summary of your Michigan physical therapy license renewal requirements. According to the Bureau of Labor and Statistics, more than 229,000 physical therapists work in the United States. Over 7,000 of those PTs work in Michigan. If you’re one of those 7,000 and looking to renew your physical therapy license in the Wolverine State, […]
Read More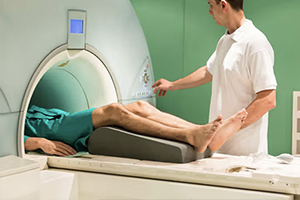







 Call
Call